A Big Picture
Weighing the Risks and Benefits of COVID Vaccination
The proliferation and increasingly easy access to COVID vaccines in America has seemingly substantiated predictions that immunization would end the virus’ pandemic level threat, though it will likely take a winter season to confirm that.
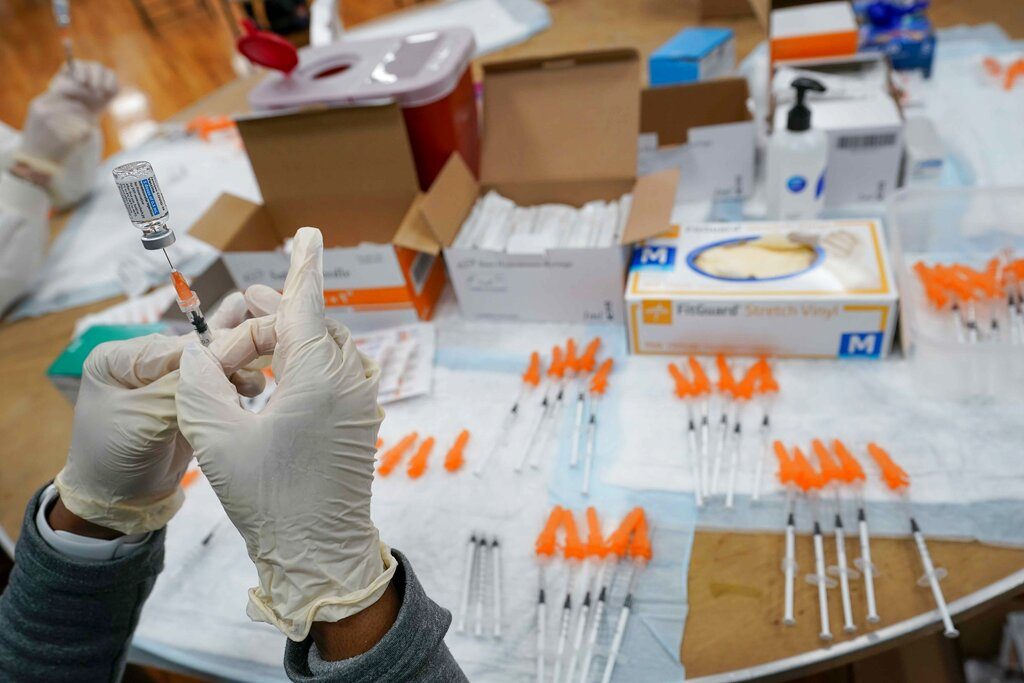
syringe with the Johnson & Johnson
COVID-19 vaccine at a pop-up
vaccination site in Staten Island, NY. (AP Photo/Mary Altaffer, File)
With nearly 3 billion doses administered worldwide and 324 million in the U.S. (counting two dose vaccines separately), another prediction has come to pass as well, reporting of new adverse side effects.
While numbers of those experiencing negative reactions remains very low, they have fed skepticism among those still wavering over whether COVID immunization presently passes their risk/benefit analysis. The question multiplies among those seen as being at lower risk, mainly people who are younger and healthy or who have already been infected with the virus.
While the U.S. is currently administering around 875,400 doses per day, a recent Monmouth University poll showed that one in five Americans remains hesitant or unwilling to take a COVID vaccine.
Risks
In the early months of the vaccine rollout, the first significant adverse reaction reported was blood clotting, a phenomenon linked chiefly to the one-dose Johnson & Johnson and AstraZeneca vaccines. Given the serious nature of the clots, the CDC and FDA temporarily paused the vaccines this past April to allow for further investigations to take place. Yet, after a review, the side effect was determined to be too rare to justify pulling the vaccines from the market. At the time, the government agencies were able to identify only 15 people (all women who, in general, are more susceptible to clotting) out of 8 million who had received the Johnson & Johnson shot. A similar determination was reached regarding the AstraZeneca vaccine, which is being distributed in different parts of the world, but not the U.S.
More recently, data have emerged about cases of myocarditis, an inflammation of the heart muscle, likely linked to the two-dose mRNA vaccines produced by Pfizer and Moderna. As of early June, some 1,200 cases of the potentially dangerous condition were reported to the nation’s vaccine safety database, mostly affecting younger males. Experts had anticipated that the complication might present itself, but the CDC said that the reported numbers were higher than expected.
Still, given that more than 300 million doses of mRNA vaccines have been administered, most experts felt the condition did not represent a high- enough risk to alter immunization guidelines.
Besides the low ratio of those experiencing the condition compared to the total vaccinated population, an additional factor holding back most doctors from any shift in vaccination recommendations is that, while myocarditis can have serious implications, studies show it as one of several long-term symptoms that can also appear in those infected with COVID.
“The way I look at these risk factors is to ask, what would happen if you are a young adult and get COVID-19 versus if you get the vaccine,” said Dr. Peter Hotez, dean of the National School of Tropical Medicine at Baylor College of Medicine and co-director of the Center for Vaccine Development at Texas Children’s Hospital. “There is a recent study of young athletes that got COVID and around 2% of them developed myocarditis in addition to others that had other cardiac and neurological issues. Young men getting myocarditis from the two mRNA vaccines was much rarer than that, something like one in 70,000, and most of those cases were self-limiting. The benefits still heavily outweigh the risks.”
The study referenced, conducted by Saurabh Rajpal, an assistant professor of cardiology at Ohio State University Wexner Medical Center, followed 1,500 college athletes (part of the same age group showing higher levels of the heart condition in response to the mRNA vaccines), 2.3% of whom showed signs of myocarditis.
The CDC emphasized that the heart-swelling cases, though requiring hospitalization in some cases, resolved themselves without significant medical treatment. Some criticized what they saw as an attempt to minimize the potential risks of the condition.
Dr. Hotez did not feel the condition was being underplayed, but that the CDC’s response reflected the big picture analysis.
“Myocarditis is serious, no question about it, but you’re still more likely to get it from COVID-19.”
Israeli researchers at the Institute of Hematology at Shamir Medical Center also recently reported what they feel is a possible connection between an increase in cases of a rare blood disorder known as thrombotic thrombocytopenic purpura (TTP) and the Pfizer vaccine. Researchers and doctors there stressed that the study group was very small and that while vaccine recipients should be vigilant of potential side effects, the study was far from producing evidence that would lead them to discourage immunization.
Dr. William Petri, professor of medicine at the University of Virginia, who is engaged in research on COVID vaccines as well as the virus’ effects on the immune system, suggested that, given the gender- specific nature of most of the adverse effects reported, recommending different vaccines to men and women in the affected age groups might be a wise approach.
“These two side effects can be avoided if women do not receive the J&J and Astrazeneca vaccines and men do not receive the mRNA vaccines. By way of contrast, one in 500 Americans has died from COVID-19,” he said.
Some would add a note to the figure of “one in 500,” that the overwhelming majority of deaths do not come from the younger men or women affected by the side effects under discussion.
Unknowns
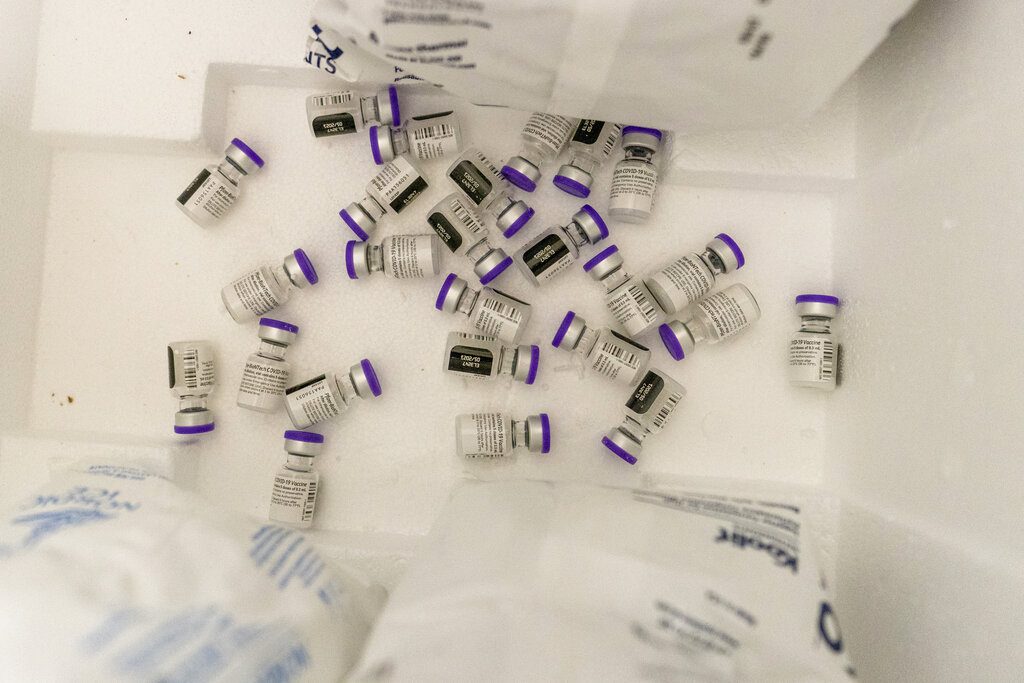
COVID-19 vaccine are seen at a
vaccination site in the Bronx,
New York. (AP Photo/Mary Altaffer)
Pharmaceutical companies, experts, and governments have proudly touted the extensive nature of the vaccine trials that combined the work of several years into one, largely as a result of massive funding from the Trump administration’s Project Warp Speed.
“If you look at the clinical trials, they were about as large as any trial gets and after almost a year of use and monitoring with multiple parallel systems this has been tracked very robustly,” said Dr. Hotez.
Still, the unknowns of what potential long-term effects could arise fueled concerns of many who remain hesitant to expose themselves to potential vaccine risks.
Dr. Petri said that the lack of significant warning signs from trial participants should be a reassuring sign.
“There is now at least seven months of follow-up from the original clinical trials without a safety signal of any longer-term side effects, so it is unlikely that a long-term side effect will appear later,” he said.
While unsupported by any scientific data, the idea that COVID vaccines could have a negative impact on fertility have been widely spread on social media, largely by sources connected to the established anti-vaccine camp.
Dr. Hotez, who has closely followed the anti-vax movement for many years and authored a book refuting many of its claims, said that the concept that COVID vaccines could cause infertility are not only wholly unsubstantiated, they are not a new accusation from those campaigning against vaccination in general.
“It wasn’t a very creative mind that put these ideas out there,” he said. “The anti-vaccine lobby has put [out] the same fake assertions about other vaccines before. They basically just copied and pasted what they said then onto COVID-19 vaccines and still with no evidence.”
Who Can You Trust?

Prior to the pandemic, the vast majority of Americans likely would have been easily won over by the near universal recommendations of the medical establishment to embrace their recommendations. Yet, after a year when many felt that the realities of the pandemic they observed did not always match with the level of alarm raised by the mainstream health establishment, and politics mixed deeply into the methods of fighting the virus, more skepticism is unsurprising.
Though wholly unconnected in substance, the Biden administration’s announcement that the intelligence community considered a lab leak to be as likely of an origin for the virus as natural evolution shook the confidence of many in unanimous expert conclusions, recalling when the idea was written off as a wild conspiracy theory by nearly all respectable voices.
Dr. Petri cautioned against conflating the issues.
“Apples and oranges,” he said. “Clinical trials in the U.S. were transparent with all the data available for scrutiny by independent experts. There is not equal transparency from the Chinese government over what happened in Wuhan.”
Dr. Harvey Risch, professor of epidemiology at Yale University’s medical school, said that while he thinks health officials were right to approve COVID vaccines for use to protect high-risk populations, that the CDC, NIH, and others were doing the public a disservice by giving what he identified as a lack of serious consideration to the risks posed to those unlikely to experience severe COVID infections.
“There is a belief that seems apparent that the medical public health regulatory establishment feels they know better about each person’s individual decision to vaccinate than the people themselves do,” he said.
In a recent opinion piece in The Wall Street Journal, he and UCLA medical school’s Professor Joseph Ladapo made the case that what has become a policy of recommending near universal vaccination for COVID should be far more nuanced for low-risk groups.
Dr. Risch felt that both data on adverse effects and the risk/benefit analysis were being distorted by much of the medical world and mainstream media.
“People are not being given credit to figure out their own risks and benefits for vaccination. It’s a sort of elitism on the part of regulatory agencies and it’s caused the public not to believe what those agencies are telling them,” he said. “It’s good that these vaccines are on the market, but there has to be much more transparency.”
The Delta Variant
A factor quickly influencing the discussion on COVID vaccination is the emergence of the delta variant, which, according to the World Health Organization, is 55 times more transmissible than older strains of the virus. The level of contagiousness, presumably demonstrated by new outbreaks in countries that had beaten the virus back, led many experts to posit that many with no immunity through vaccination or COVID recovery will likely contract this variant before long.
The emergence of more contagious variants in general has been a public health argument for mass vaccination as such strains are more likely to develop when the virus can roam free among large populations. Additionally, the heightened risk of contraction many feel is yet another factor that should push more people to get vaccinated.
Yet, a complicating factor is emerging: data implying that the delta strain can beat several of the vaccines in use, as evidenced by outbreaks in Israel and England, where vaccination rates are very high.
Moderna is the one vaccine version that seems most effective against the variant, with blood samples showing that it causes the bodies of vaccinated people to produce antibodies against this strain as well.
While there is a mounting number of vaccinated people who have tested positive for the delta variant, early data show most cases to be asymptomatic or very mild.
A study done in May by Public Health England, showed that the Pfizer vaccine was 88% effective against symptomatic cases caused by the new strain and showed even higher rates of preventing severe outcomes.
The Scales

The value of vaccination for those at high risk for hospitalization and serious disease form COVID is widely accepted.
Yet, much hesitancy remains among younger people, who overwhelmingly fare much better with the virus. Still, most experts are strongly encouraging all those eligible to vaccinate, backed by a wide array of government-sponsored incentive programs.
Some have used young people’s potential role in spreading the virus to at-risk populations as a key motivating factor.
Dr. Hotez said that the risks themselves should be enough to convince younger people to vaccinate.
“Even if they don’t get seriously ill, you still have to worry about long-term COVID-19 effects like neurological issues, brain fog, and others, which could keep you from functioning at a high level for quite a while,” he said.
As reinfection has remained very uncommon and those who have re-contracted the virus rarely suffered serious cases, some who already had COVID are also among those who are not rushing to vaccinate. Their feelings seem supported by emerging scientific data showing that the body continues to recognize and retain the tools to fight off the virus long after recovery.
One such study conducted by a researcher at the University of Washington showed that while initial antibodies often receded within a few months, bone marrow testing showed that memory B cells remained in the blood that would likely fight off infection for years (at least against strains similar enough for them to “remember”).
Dr. Hotez said that the lack of uniform responses still made vaccination the best option for recovered COVID patients.
“The problem is that while there is some immunity, it’s variable depending on the antibody level, so we don’t know whether a person will have long-term protection or not,” he said.
Dr. Hotez went on to quote one of several recent studies showing that those who have recovered from COVID and also take the vaccine have the highest levels of protection.
Stressing his message that individuals should be given what he sees as fairer tools to evaluate whether vaccination is the best option for them, Dr. Risch criticized what he labeled as a “misrepresentation” of virus risks for younger people.
“There is a message that everybody out there is at a huge amount of risk from COVID, but the stratification of risk of serious outcomes and death are 1,000-fold when you compare people in the lowest risk groups to the higher ones, which mostly has to do with age and chronic conditions like diabetes. But people under 60 without conditions survive pretty well. A small fraction do get chronic symptoms that can be managed,” he said.
Some of what Dr. Risch called “fearmongering” over the virus also came from much of the medical establishment’s reticence to acknowledge the effectiveness of therapeutics that have been successful in mitigating serous outcomes if applied early in the onset of infection.
“There are people who are at high risk from COVID infections and there are those who are not,” he said.
“If the medical establishment and regulatory bodies want to be trusted, they need to be open about the facts and give people the tools they need to make their own decision.” n
To Read The Full Story
Are you already a subscriber?
Click "Sign In" to log in!

Become a Web Subscriber
Click “Subscribe” below to begin the process of becoming a new subscriber.

Become a Print + Web Subscriber
Click “Subscribe” below to begin the process of becoming a new subscriber.

Renew Print + Web Subscription
Click “Renew Subscription” below to begin the process of renewing your subscription.




